For Healthcare Providers
Partner with us to provide your patients with advanced hyperbaric and wound care services. Our streamlined referral process makes it easy to get your patients the specialized care they need.
Emergency Hyperbaric Referrals
For the following emergency indications, please call us directly at 802-HEALING (802-432-5464) for immediate consultation.
- Carbon Monoxide Poisoning: Acute intoxication, especially with severe symptoms
- Decompression Sickness (DCS): "The bends"
- Air or Gas Embolism
- Gas Gangrene (Clostridial Myonecrosis)
- Necrotizing Soft Tissue Infections
- Acute Traumatic Ischemia: Crush injuries, compartment syndrome, and acute arterial insufficiency
- Compromised Skin Grafts and Flaps
- Severe Acute Blood Loss Anemia: Used when blood transfusion is not possible
- Central Retinal Artery Occlusion
- Intracranial Abscess
Why Refer to Green Mountain?
We make it easy for you to refer patients who need specialized wound care or hyperbaric oxygen therapy. Our team works closely with referring physicians to ensure seamless care coordination.
- Quick and easy referral process
- Same-day or next-day appointments available
- Comprehensive evaluation and treatment planning
- Regular progress reports to referring physicians
- Coordination with your patient's care team
- Direct line of communication with our specialists
Services Available
- Hyperbaric oxygen therapy (HBOT)
- Chronic wound management
- Diabetic foot care
- Vascular wound assessment
- Acute wound care
- Diagnostic vascular studies
Direct Contact
Why HBOT Works: The Science
Hyperbaric oxygen therapy leverages fundamental physiological mechanisms to enhance tissue healing and combat infection.
Hyperoxygenation via Henry's Law
At 2.0–2.5 ATA, oxygen dissolves directly into plasma in large amounts—enough to meet tissue metabolic demand even without hemoglobin. This improves oxygen delivery even in areas with poor perfusion, edema, or microvascular compromise.
Enhanced Tissue Diffusion
HBOT increases the diffusion gradient, allowing oxygen to penetrate farther from capillaries into ischemic zones. Critical for diabetic foot ulcers, radiation necrosis, and compromised grafts/flaps.
Angiogenesis & Neovascularization
Intermittent hyperoxia–normoxia cycling triggers VEGF upregulation, endothelial progenitor cell mobilization, and capillary budding—resulting in permanent microcirculation improvement over weeks.
Fibroblast & Collagen Synthesis
Oxygen is essential for proline and lysine hydroxylation (collagen cross-linking) and fibroblast proliferation. HBOT restores oxygen tension to enable stronger granulation tissue and better wound closure.
Enhanced Leukocyte Killing
Neutrophils require oxygen for the oxidative burst (NADPH oxidase). HBOT restores leukocyte function in hypoxic tissue, enabling better control of infection—especially anaerobic infections.
Direct Antimicrobial Effects
High oxygen levels are directly toxic to obligate anaerobes (e.g., Clostridium perfringens) and inhibit toxin production. Key for gas gangrene and necrotizing soft tissue infections.
Edema Reduction
Hyperoxia causes arteriolar vasoconstriction while maintaining tissue oxygenation. This decreases capillary leak, reduces compartment pressures, and improves microvascular flow in crush injuries.
Antibiotic Synergy
HBOT improves antibiotic penetration into hypoxic tissue and enhances activity of aminoglycosides and quinolones. Especially useful in refractory osteomyelitis and chronic diabetic infections.
Stem Cell Mobilization
HBOT stimulates bone marrow release of stem/progenitor cells into circulation. Studies show up to an eight-fold increase over a full treatment course, enhancing endogenous tissue repair and regeneration in ischemic and injured tissues.
Evidence-Based Indications
The Undersea and Hyperbaric Medical Society (UHMS) recognizes 17 approved indications for HBOT, with strong evidence supporting its use in:
Materials Today | September 2025
Multimodal Approaches for Enhanced Wound Healing
A comprehensive review of chemical and physical strategies for chronic wound management
6.5M
Patients affected by chronic wounds annually
25%
Lifetime risk of DFU in diabetic patients
Multimodal Wound Healing Framework
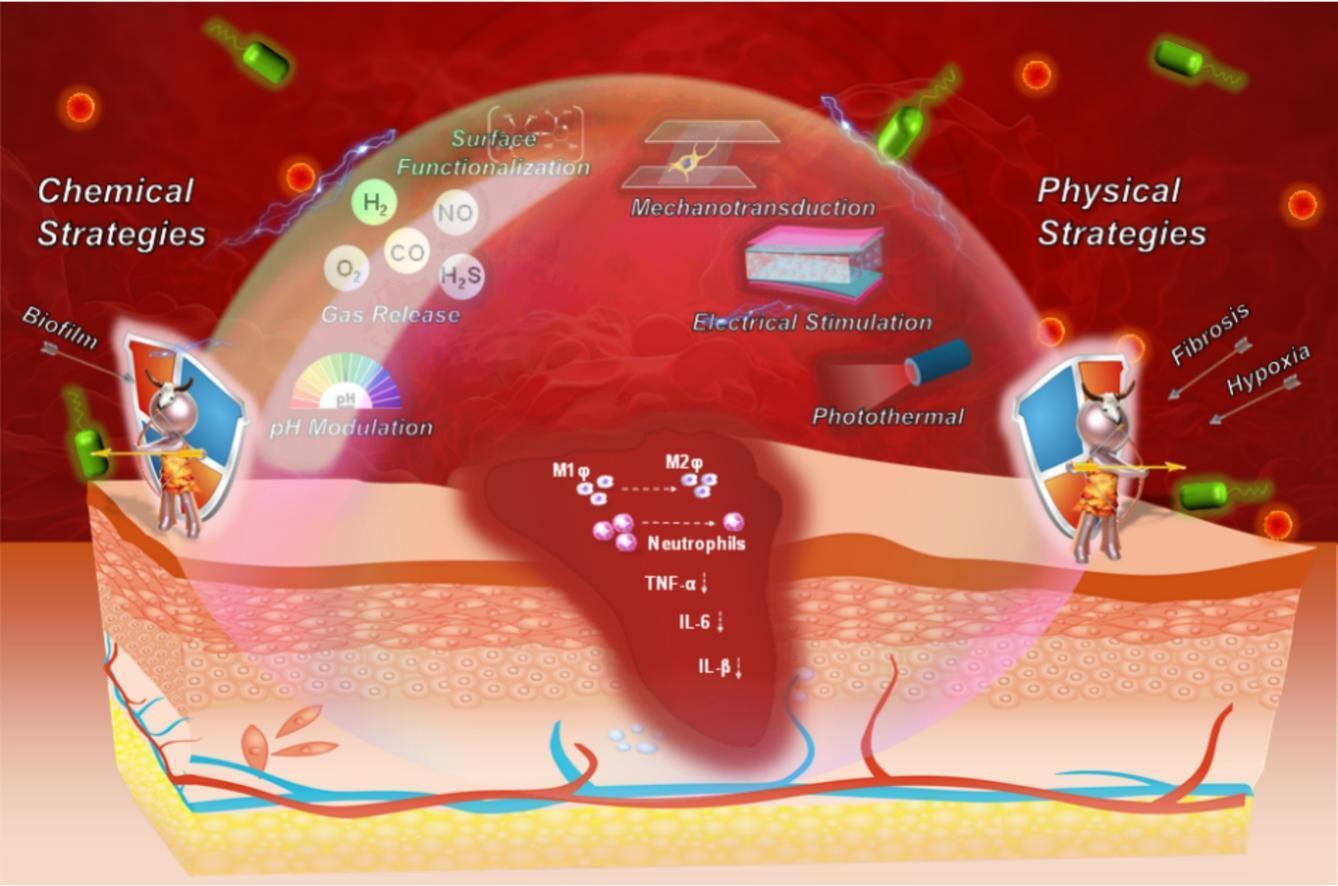
Figure: Synergistic integration of chemical and physical strategies can regulate inflammation, promote angiogenesis, and enhance extracellular matrix remodeling.
The Chronic Wound Challenge
Chronic wounds remain trapped in a prolonged inflammatory state, characterized by:
- •Biofilm formation — polymicrobial interactions resist host immunity
- •Elevated proteases (MMPs) — damage ECM and growth factors
- •Excessive ROS — induce cellular senescence and impair healing
- •Down-regulated receptors — EGFR and TGF-β receptors impaired
Traditional wound care provides symptomatic treatment but often fails to re-establish normal healing cascades. Multimodal approaches combining chemical and physical strategies show promise in breaking the deleterious cycle.
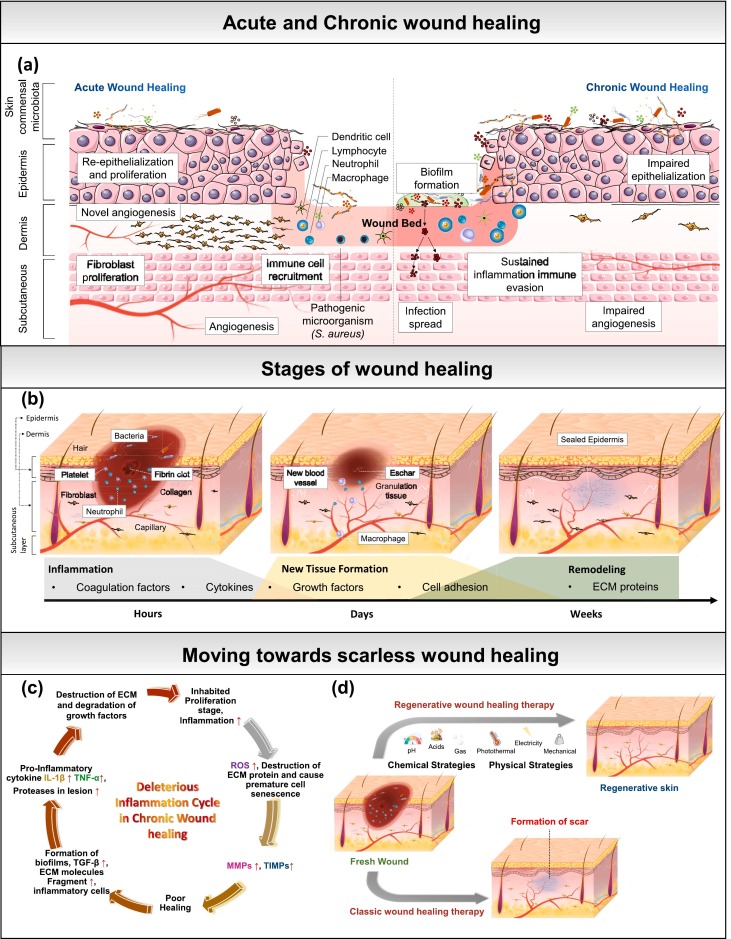
Figure 1: (a) Acute vs chronic wound progression. (b) Three phases of wound healing. (c) Deleterious cycle of chronic wounds. (d) Chemical and physical strategies for regeneration.
Gas-Mediated Therapies: Molecular Mechanisms
Gasotransmitters (GSMs) play critical roles in wound healing. Diabetic wounds often exhibit deficiencies in one or more GSMs, suggesting exogenous delivery may enhance outcomes.
Nitric Oxide (NO)
Mechanisms: Antimicrobial, anti-inflammatory, provascular
Effects: ↑ Angiogenesis, ↓ Apoptosis, ↓ Inflammation, ↑ Cell division
Pathways: NO/cGMP/FOXG1, Akt/CREB, sGC/PKG/iNOS
Hydrogen Sulfide (H₂S)
Mechanisms: Antimicrobial, anti-inflammatory
Effects: ↑ Vascular repair, ↓ Apoptosis, ↑ Mitochondrial function
Pathways: PI3K/Akt/GSK-3β, eNOS/NO/cGMP, Nrf2/ARE
Oxygen (O₂/HBOT)
Mechanisms: Anti-inflammatory, provascular, ECM remodeling
Effects: ↓ Apoptosis, ↑ Proliferation, ↓ Oxidative stress
Pathways: HIF-1α↑, p38MAPK/Nrf2, IL-6/STAT3
Carbon Monoxide (CO)
Mechanisms: Antimicrobial, anti-inflammatory, immunomodulatory
Effects: ↑ Angiogenesis, ↑ Stem cell homing, ↓ Neuroinflammation
Pathways: HO-1/CO, VEGF↑, PI3K/Akt/mTOR
Clinical Note: Hyperbaric oxygen therapy (HBOT) at 2.0–2.5 ATA activates HIF-1α/SDF-1α signaling, p38MAPK/Nrf2 pathway, and modulates IL-6/STAT3 to promote tissue repair.
Physical Strategies for Tissue Regeneration
Photothermal Therapy (PTT)
NIR light induces localized heating that enhances cellular metabolism, reduces inflammation and promotes collagen organization. Effective for bacterial eradication and cellular stimulation.
Electrical Stimulation
Piezoelectric and triboelectric stimulation enhances cell migration, proliferation, and tissue regeneration through modulation of cellular signaling pathways.
Mechanotransduction
Controlled mechanical stimuli (stretching, compression) influence cellular behavior and ECM organization to reduce excessive collagen deposition and scarring.
Clinical Implications: Toward Multimodal Treatment
Key Findings
- • Single-modality approaches often insufficient for chronic wounds
- • Synergistic combinations enhance therapeutic efficacy
- • HBOT + biomaterial scaffolds show enhanced angiogenesis
- • Gas therapy + electrical stimulation accelerates epithelialization
Treatment Considerations
- • Assess wound microenvironment (pH, oxygenation, biofilm)
- • Consider patient comorbidities (diabetes, vascular disease)
- • Combine modalities based on wound etiology
- • Monitor for optimal treatment timing and sequencing
Source: Nahak BK, et al. Materials Today. 2025;88:1087-1125. doi: 10.1016/j.mattod.2025.07.009
Read Full ArticleProvider Referral Form
Submit a referral and we'll contact you soon.
Questions About a Referral?
Our team is happy to discuss whether a patient would benefit from our services.
Call Us: 802-HEALING