Platelet-Rich Plasma (PRP) Therapy
Harness your body's own healing power. PRP concentrates growth factors from your blood to accelerate wound closure and tissue regeneration for chronic, non-healing wounds.
What is Platelet-Rich Plasma?
Platelet-Rich Plasma (PRP) is an autologous therapy — derived entirely from the patient's own blood — that concentrates the platelets, growth factors, and healing proteins your body naturally uses to repair tissue.
When a chronic wound stalls in the inflammatory phase, PRP can restart the healing cascade. The concentrated growth factors modulate inflammation, stimulate new blood vessel formation (angiogenesis), promote collagen synthesis, and provide a fibrin scaffold for new tissue to grow onto.
Originally developed for orthopedic and sports medicine applications, PRP has emerged as a powerful tool in wound care — particularly for complex, recalcitrant wounds where standard therapies alone haven't been enough.
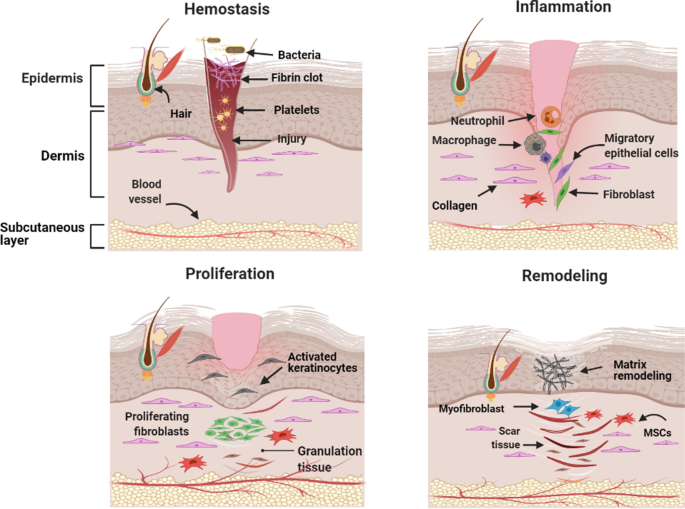
The four phases of wound healing — PRP helps restart stalled processes
Autologous & Safe
PRP is derived from the patient's own blood, minimizing risk of allergic reaction or rejection.
Concentrated Growth Factors
Contains cytokines, chemokines, and growth factors that jump-start the healing cascade.
Promotes Angiogenesis
Stimulates the formation of new blood vessels to deliver oxygen and nutrients to the wound.
Accelerates Closure
Meta-analysis of 1,952 patients showed PRP increased complete wound closure rates in diabetic ulcers.
How PRP Treatment Works
PRP preparation and application is performed in-clinic and is well-tolerated by patients. The entire process typically takes less than an hour.
Blood Draw
A small sample of the patient's blood is collected — similar to a routine lab draw.
Centrifuge Processing
The blood is spun in a centrifuge to separate and concentrate the platelet-rich plasma layer.
Wound Preparation
The wound is cleansed and gently debrided to create an optimal environment for PRP application.
PRP Application
The concentrated PRP is applied directly to the wound bed — injected around the wound margins and/or applied as a topical gel.
Follow-Up Care
A protective dressing is applied, and regular follow-up visits monitor healing progress.
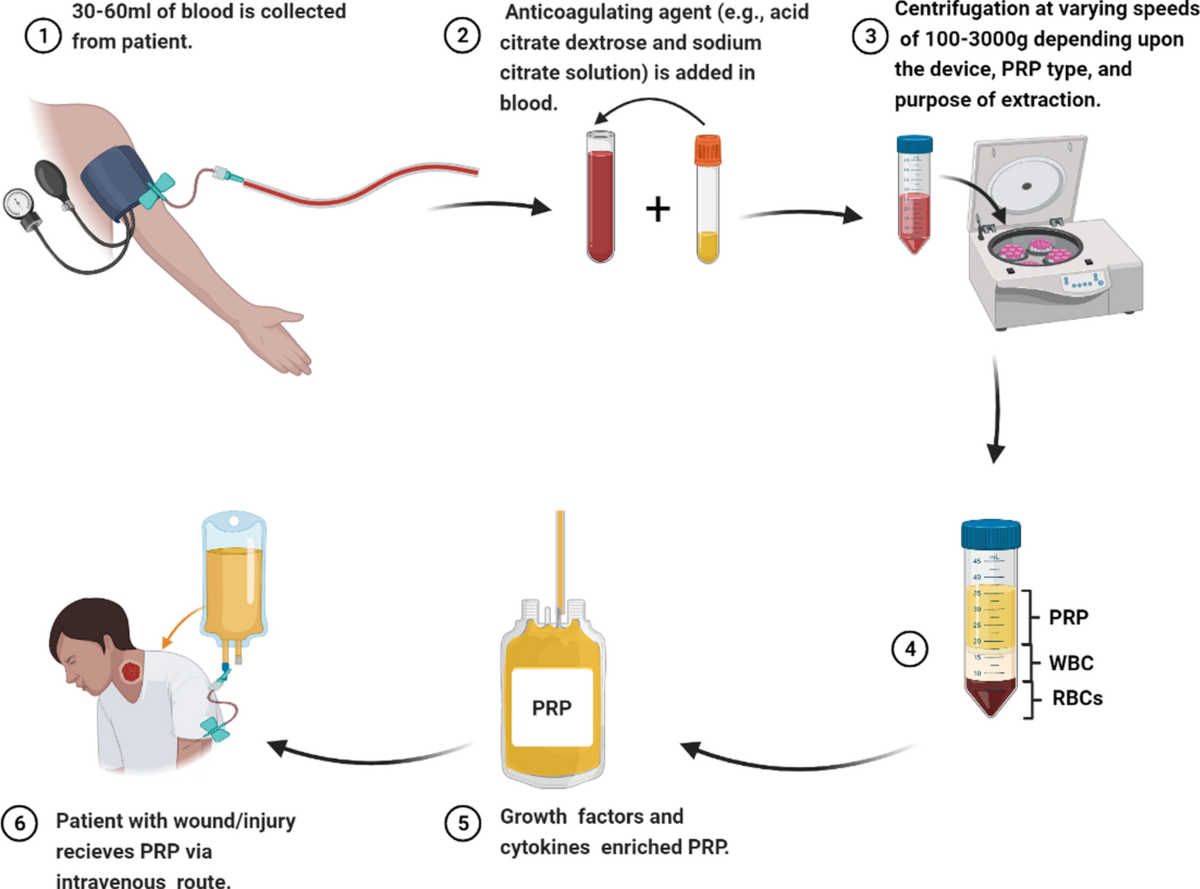
The PRP preparation and application process
How PRP Promotes Healing at the Cellular Level
Activated platelets release growth factors that recruit stem cells, stimulate angiogenesis, and promote tissue regeneration.
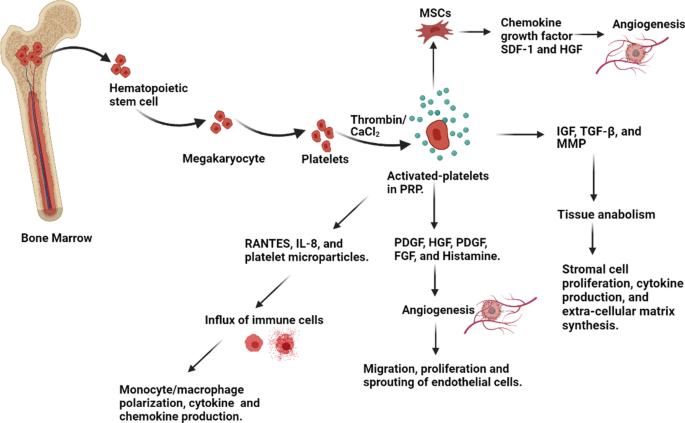
Platelet activation cascade and downstream healing pathways
Conditions Treated with PRP
PRP is particularly effective for chronic wounds that have stalled in the healing process. It can jumpstart healing in cases that might otherwise progress toward amputation or prolonged suffering.
- Chronic non-healing diabetic foot ulcers
- Lower-extremity venous ulcers
- Pressure injuries (pressure ulcers)
- Recalcitrant wounds unresponsive to standard care
- Post-surgical wounds with delayed healing
- Complex or atypical wounds
Why PRP for Wound Care?
When a chronic wound refuses to heal, it's often because the body's natural repair process has stalled. PRP delivers a concentrated dose of the very growth factors needed to restart that process.
PRP can be applied topically as a gel or injected peri-wound. It empowers clinicians to harness the patient's own biology in the fight against chronic wounds.
This isn't just innovation for innovation's sake — it's a practical, evidence-supported approach that expands treatment options and improves outcomes.
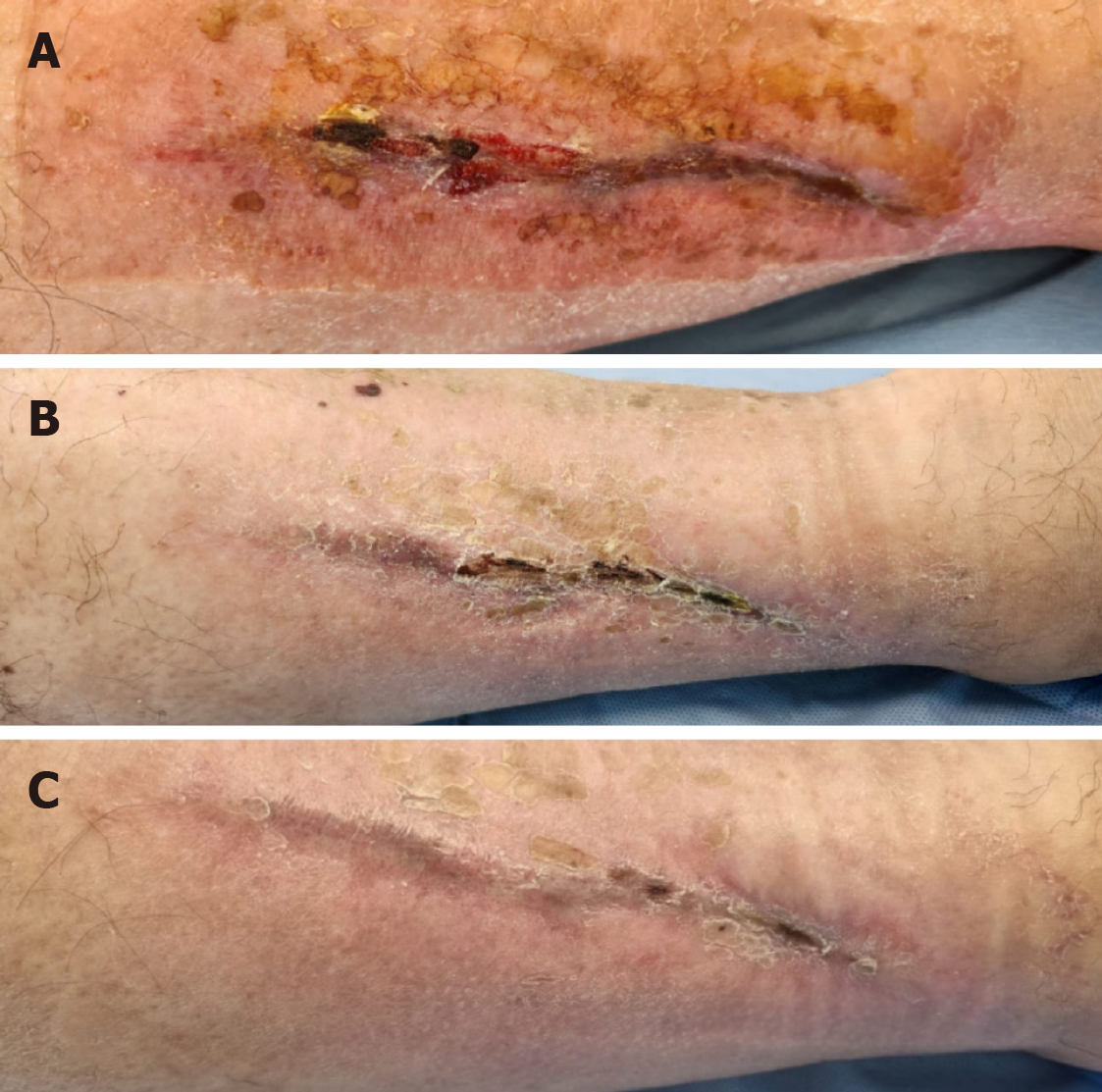
Wound healing progression with PRP therapy
Research & Evidence
PRP for wound care is supported by a growing body of clinical evidence, including randomized controlled trials and meta-analyses.
Regenerative Therapy (2026)
Systematic review of 17 studies across 12 databases produced 27 evidence-based recommendations for PRP in chronic wounds, confirming its role as an effective adjunctive therapy with strong evidence for venous ulcers.
View SourceMedicina (2025)
Comprehensive review confirms PRP significantly enhances healing in non-healing diabetic foot ulcers — particularly when combined with debridement or skin grafting — by promoting angiogenesis, reducing inflammation, and providing antimicrobial properties.
View SourceMayo Clinic Proceedings (2021)
Meta-analysis of 20 randomized controlled trials and 5 observational studies on 1,952 patients found PRP increased complete wound closure, sped healing, and reduced wound size in lower-extremity diabetic ulcers.
View SourceCureus (2018)
Observational study of 104 participants with chronic wounds treated with PRP injections showed 82% of patients achieved complete healing by the 10th treatment visit.
View SourceJournal of Functional Biomaterials (2018)
PRP supports endothelial and epithelial regeneration, promotes angiogenesis and collagen formation, and provides a fibrin scaffold for new tissue growth.
View Source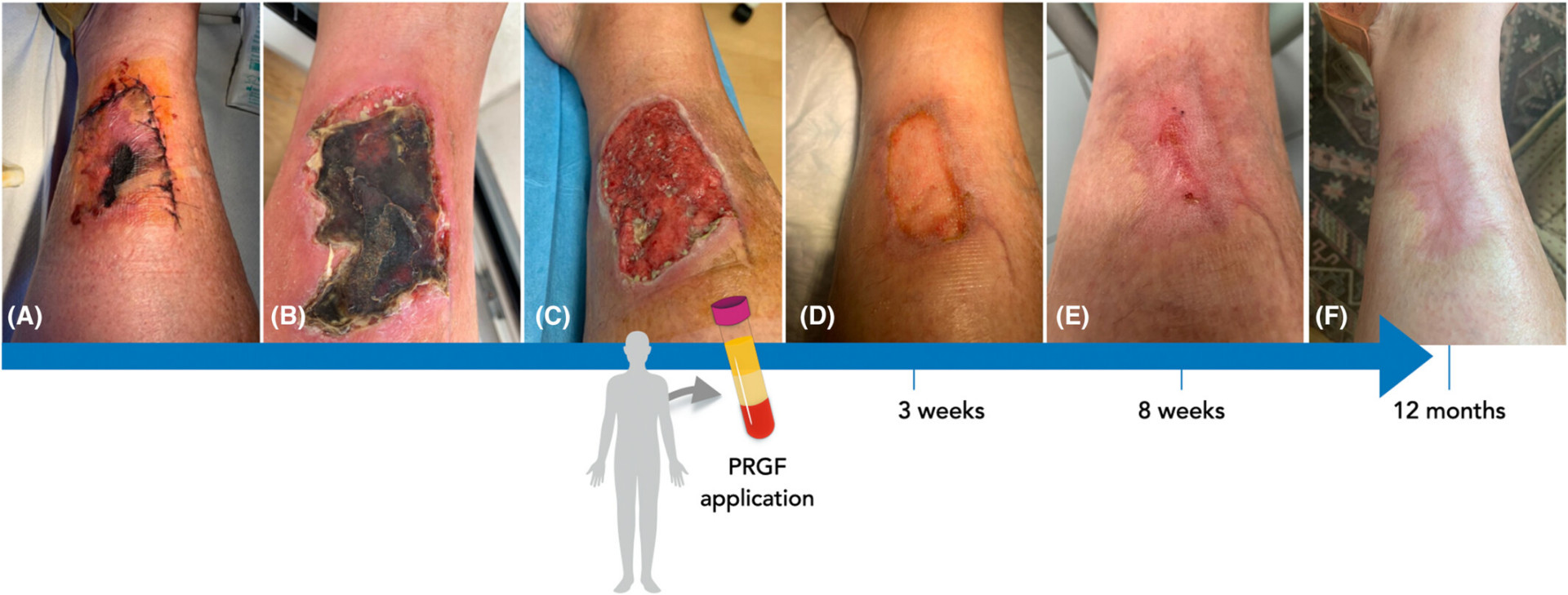
Clinical case: wound healing timeline following PRP (PRGF) application
Is PRP Right for Your Wound?
If you have a chronic wound that hasn't responded to standard treatments, PRP therapy may help accelerate your healing. Schedule a consultation to learn more.
